Frank Llosa, CEO and founder of KetoneAid Inc., and self-educated expert on all-things ketone. We dive into the discussion with a history of how Frank ended up an innovator and field leader in a biological product when his career and formal education were in startups and finance. Tune in to hear about the products on offer from KetoneAid (KE4, K1,3, and KE1) and the science behind each of them. From breaking down the pioneering research on ketones by Dr. Richard Veech to discovering alternatives to ethanol-based alcohol, Frank walks us through the history of ketone research and the biochemistry involved.
Sharpness Sustained with KetoneAid
By: Ariel Kamen, BSN, RN
High performers have been searching for the perfect human fuel to sustain their ninja-focused states. Human metabolic pathways produce energy through either sugar or fat breakdown. Glycolysis uses sugar for fuel while ketosis uses fat for fuel. With Frank Llosa, we learn that ketone bodies are a more efficient fuel than glucose (Prince, Zhang, Croniger, & Puchowicz, 2013). On Episode 36 of the KnowYourPhysio podcast, Andrés Preschel facilitates our discussion of ketone power made practical, how to get into ketosis effectively, and ketone salts versus ketone esters.
Perceptions surrounding ketosis are typically related to fat loss and to clarify, ketosis is not a diet— it’s a metabolic state. Yes, ketosis is best achieved using nutrition, but to understand the significance of its energy production we have to take on a physiologic lens. In this article we will take a peak at both benefits and risks of existing in a fat-burning ketogenic state.
Ketone Bodies
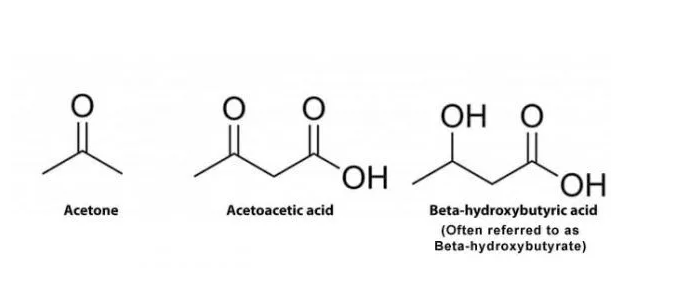
Ketone bodies, such as R-b-hydroxybutyrate (BHB) and acetoacetate (AcAc), are alternate energy substrates to glucose that are utilized by the brain and tissue especially during early development. Under conditions of reduced glucose availability, such as starvation, fasting, heavy exercise, and strict caloric intake of a high fat/low-carbohydrate diet (Evans, Cogan, & Egan, 2017), d-β-hydroxybutyrate and acetoacetate are derived and metabolized. (Abdul, Clarke, Evans, 2020). Imagine ketone bodies being the juice within a battery while the battery itself is the mitochondria.
Ketosis as a Metabolic State
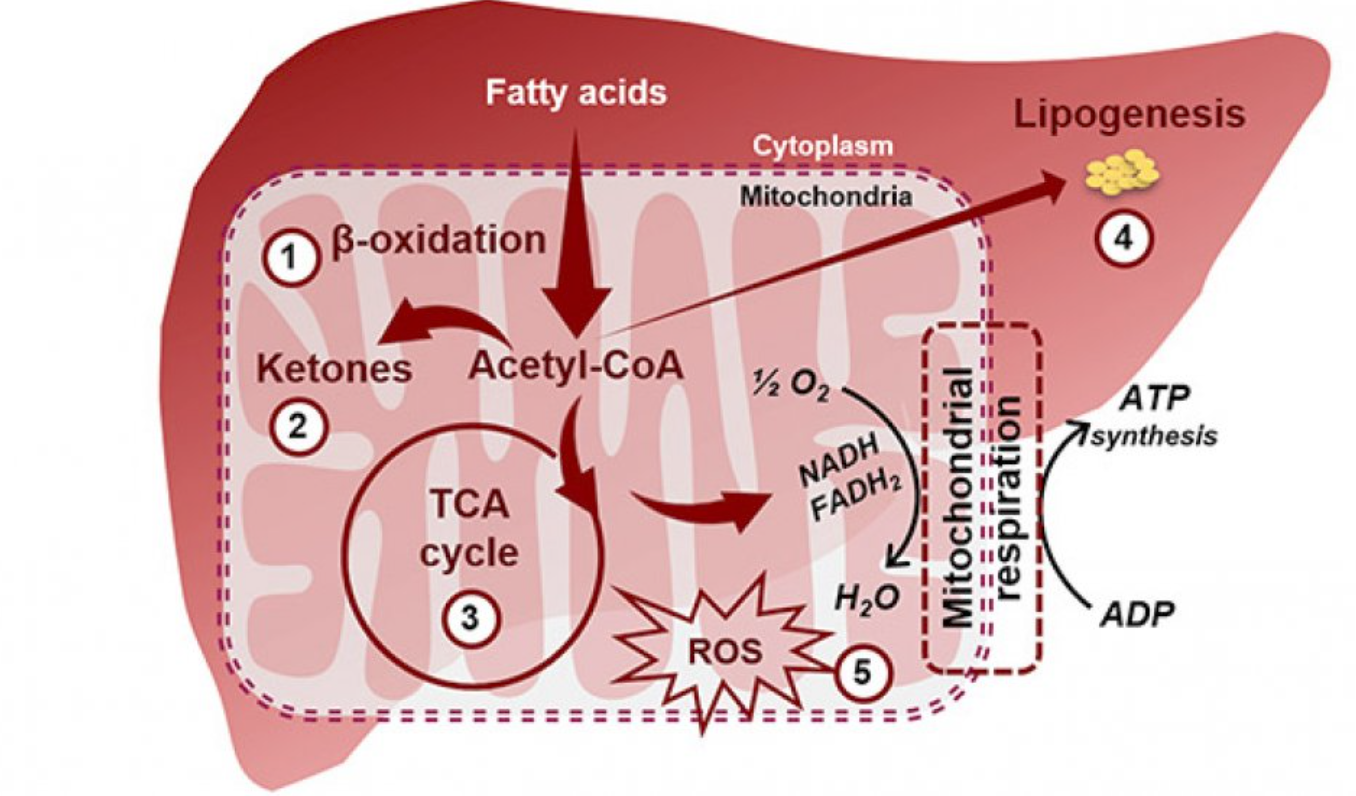
Our vital organs (i.e. heart and brain) are lipophilic, meaning they prefer to use fat for energy. Within every organ there are mitochondria which produce the energy that is used by the entirety of the organ and organism. Disorders where the body is unable to metabolize fat correlates with the development and progression of heart failure (Katsiki, Doumas, & Mikhailidis, 2016).
The last thing we want is our throbbing hearts to fail, emphasizing the importance of incorporating dietary fats and being able to metabolize ketone bodies.
In the presence of both glucose and fat, the body prioritizes the metabolism of glucose. Glucose signals the liver towards lipogenesis–storing fat as adipose tissue to be used later. Fat storage is a natural and protective physiological function, but can be a limitation to health optimization when enough energy is exerted to use up the stores.
Lack of physical activity of either fuel sources manifests as weight gain and eventually obesity if sedentation is sustained. Could it be that obesity stems from a life of inactivity? Fatty foods are not necessarily the issue when a person isn’t exercising.
Ketosis is the metabolic state of burning fat for fuel. Normally, the brain metabolizes glucose for cognitive function, but in glucose-sparse condition brain imaging studies support the notion of enhanced brain energy metabolism with ketones (Jensen et al. 2020). Further evidence suggests that ketosis as a metabolic state enhances athletic performance, cognition and aids in recovery (Napoleão, Fernandes, Miranda & Marum, 2021). Each time we consume food or drinks, we have control over the metabolic pathway our liver will favor.
Ketogenic Sleep
Sleep is an evolutionary mechanism of the body to rest and repair for the upcoming day ahead. Without sleep, energy, metabolism and cognitive function fade. Neurocognitive abilities are essential for humans to interact with their surrounding environment, and acquiring these abilities is a progressive process (Altayyar, Nasser, Thomopoulos & Bruneau, 2022). Without sleep, we will not progress, we will not evolve.
The recipe for enhanced sleep is multifaceted with considerations of breath work, light exposure, nutritional intake, and time. For our purpose here, we will take a closer look into the role ketosis has on enhanced sleep.
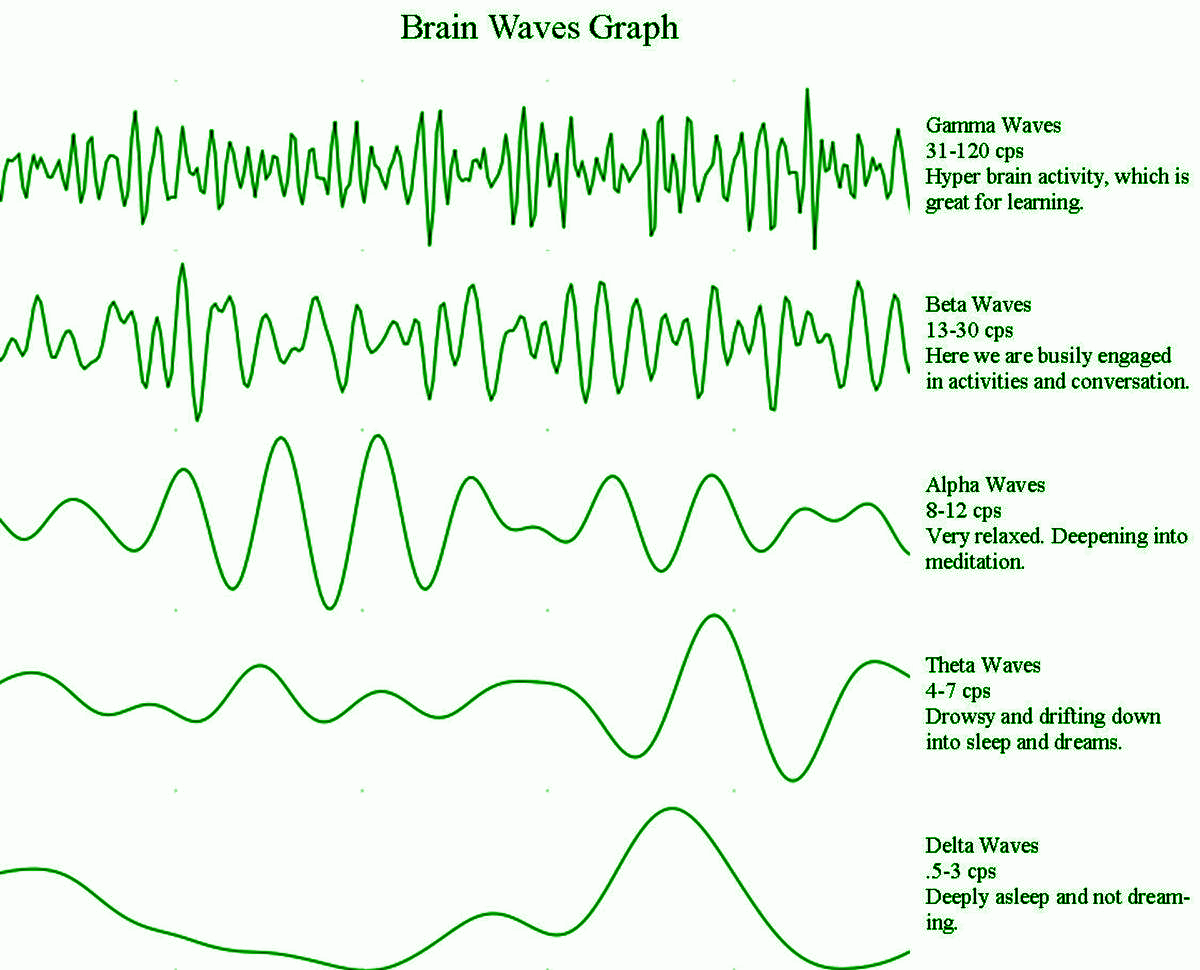
Sleep occurs in a cyclic pattern divided into four stages. As the brain relaxes into the slowest oscillation, called delta wave deep sleep, the brain is able to focus on tissue repair, immune processes, energy restoration, and memory retention by storing neural networks into the hard drive of the brain – the hippocampus, for later access. Without experiencing this stage, growth and development are heavily impaired. Sleep efficiency is correlated to the amount of time spent in delta wave sleep (Gao et. al, 2020). This makes sense because it is during delta wave sleep that our body repairs itself through a process called autophagy.
Sleep to Clean
Autophagy (auto-self; phagy-eating) is the molecular process of our cells eating their junk counterparts and using that energy to produce newly functioning cells. This process prevents cellular damage and promotes survival in the event of energy or nutrient shortage (Dikic & Elazar, 2018). Complete digestion of faulty cells are important to avoid inflammatory cascades that may lead to vital organ failure (Yamaguchi, 2019). The mechanistic target of rapamycin (mTOR) is the signaling pathway that coordinates environmental and intracellular cues to control cell growth.
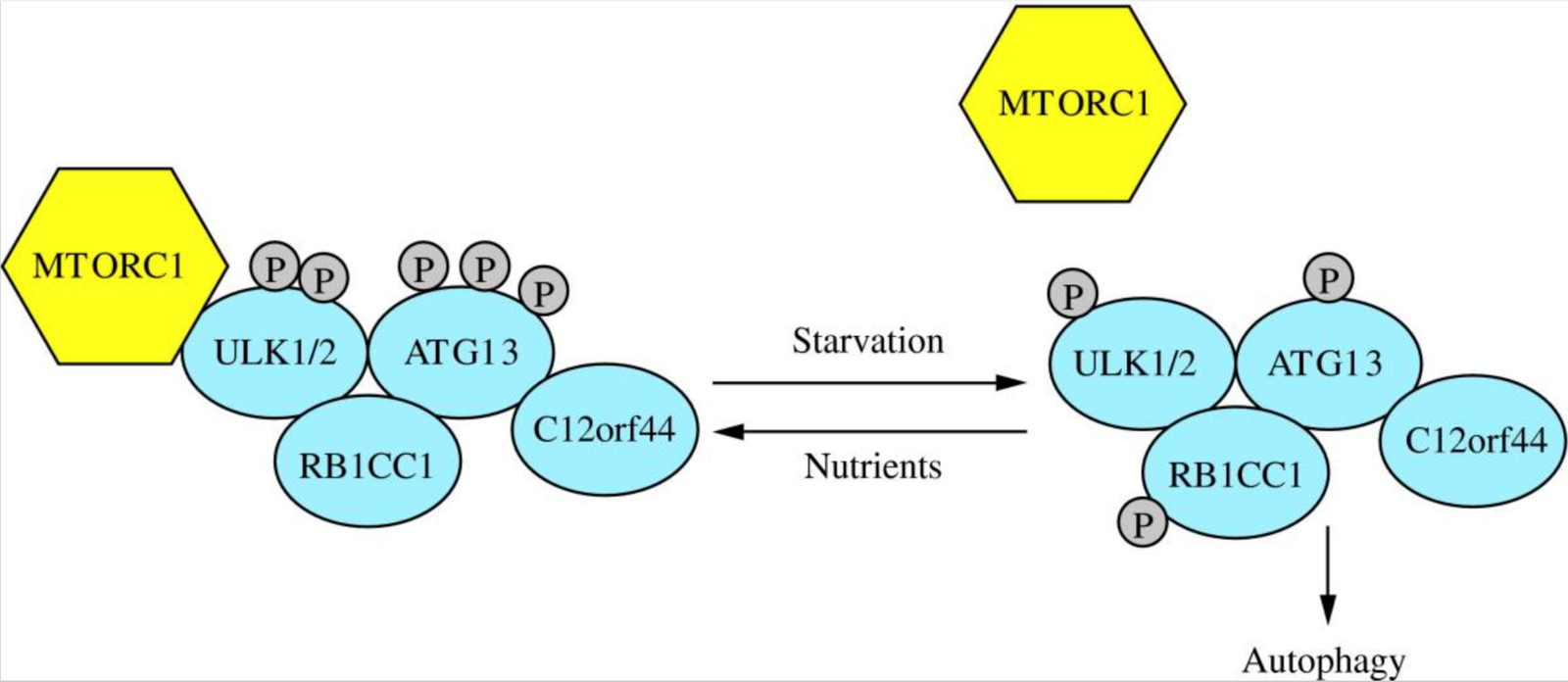
mTOR complex 1 (mTORC1) has an established role in regulating metabolism, translation, and autophagy. The start of mTORC1 signaling is directly related to nutrition status. During starvation or ketogenic states, mTORC1 dissociates from the complex which allows the complex to induce autophagy (Condon & Sabatini, 2019).
Although Frank Llosa was uncertain about the science behind improved recovery scores, Andres Preschel and his KYP team took a closer look into the physiology of ketone bodies and mTORC1 signaling to perform autophagic processes as rationale behind improved sleep scores after ingestion of KetoneAid’s KE4, Ketone Ester.
Sleep Hormones
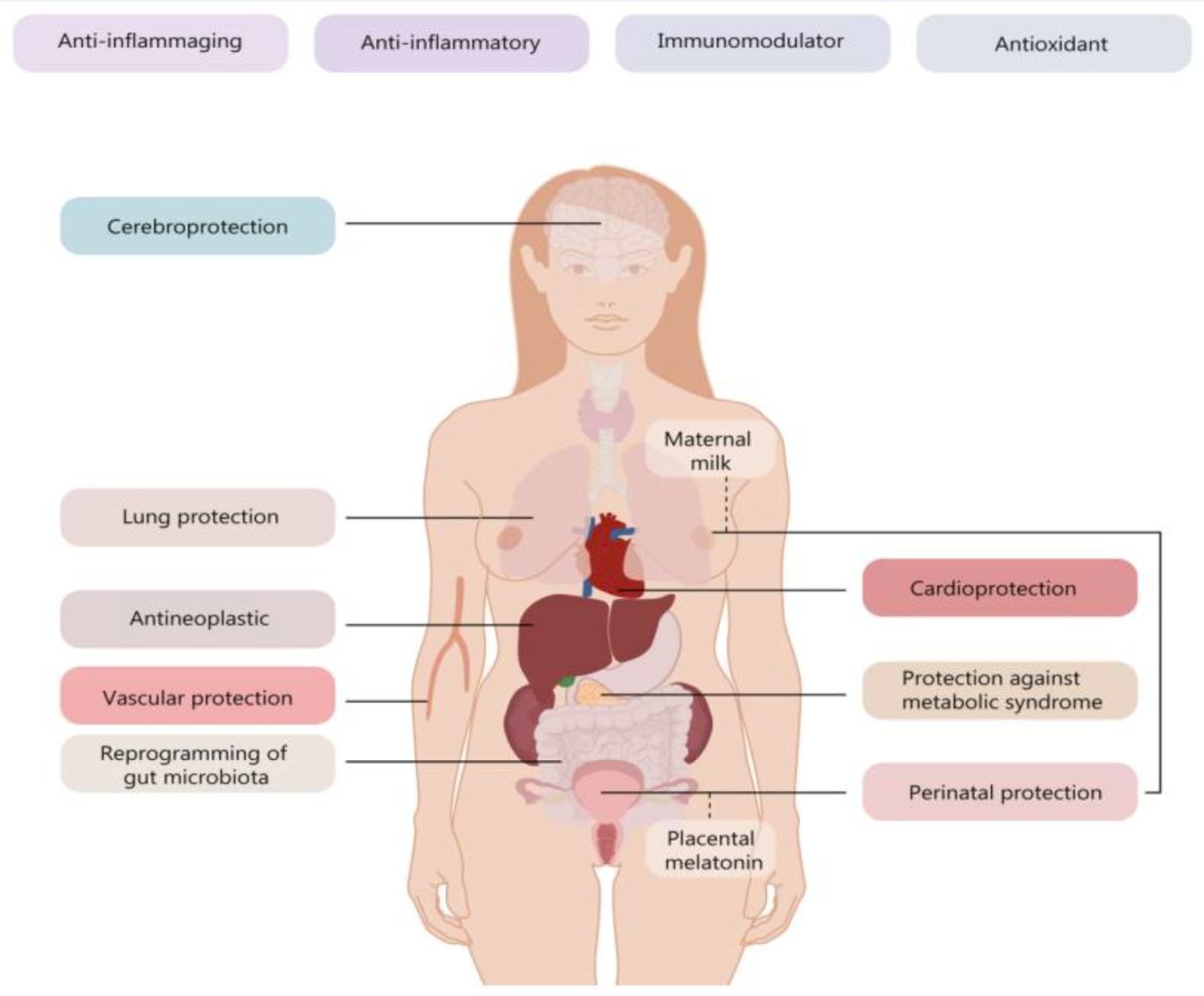
Melatonin is the sleep hormone released by the pineal gland. On a cellular level, melatonin functions in all cells and organs to induce sleep as well as aid in cellular cleaning. We can think of melatonin like soap – circulating within the bloodstream scrubbing away all of the toxins and foreign pathogens that may negatively impact our body and mind for the upcoming day. The widespread effects of melatonin on the body are depicted in the diagram below (Chitimus et. al, 2020).
Production of melatonin can either occur naturally in the brain and gut or with external supplementation. Ingesting oral melatonin suppresses the brain and body of their natural ability to release melatonin into circulation. Supplementation of melatonin should be done with extreme caution and understanding that melatonin release is further suppressed due to a decrease in pineal size as part of the natural aging process (Tan, Xu, Zhou & Reiter, 2018). To promote longevity, it is suggested that exercising endogenous melatonin secretion is preferred over oral supplementation.
In 2013, it was first published that insulin and melatonin are antagonists (Peschke, Bähr & Mühlbauer, 2013). This means the presence of insulin in the bloodstream dominates over the amount of melatonin. More melatonin in the bloodstream will allow for thorough cleaning and sustained sleep. Eating carbohydrates before bed is a recipe for poor quality sleep because the ingestion of glucose causes the release of insulin. Food choices in the hours before bedtime must be wisely selected in order to activate autophagy via the mammalian target of rapamycin.
Ketogenic Diet
Burning fat for fuel begins when the liver is depleted of all its sugar storage. The minimum amount of carbohydrates needed to prevent tissue wasting and ketosis is 50 to 100 g/day (Porth, 2011). In order to desolate sugar from the body, consumption of <50G of carbohydrates per day is required to prevent insulin release. By simultaneously increasing intake of eggs, meat, fish, heavy creams, and nuts while decreasing intake of grains, rice, quinoa, fruit, and vegetables, the metabolic scale is tipped into a fat burning state.
The Ketogenic Diet is not a quick fix and is formally designed to be executed over a span of multiple months. It is dangerous to rapidly flip the metabolic switch because of the associated sugar withdrawal that coincides with decreasing carbohydrate intake (DiNicolantonio, O’Keefe & Wilson, 2018). It is best to start by changing each meal one at a time. It will take time and consistency for a person who eats a bagel each morning for breakfast every morning to feel satiated by anything other than that bagel.
Implementing the Ketogenic Diet must be done with adequate hydration because the risk of developing kidney stones is inherently higher (Yılmaz et. al, 2021). Uric acid stones are the most prevalent kidney stones in patients on ketogenic diets followed by calcium-based stones (Acharya et, al. 2021). Low urinary volume related to dehydration is a relevant etiology of uric acid stones, making hydration an absolute priority when on the Ketogenic Diet (Ma et. al, 2018). To avoid neuroendocrine dysfunction, it is recommended that both men and women consume >1.8L of water daily. (Armstrong & Johnson, 2018). This is equivalent to 4 standard size water bottles. Not only is hydration important for its protection against kidney stones, but it is also vital to maintain adequate cardiac output through preload by increasing the volume within the vasculature.
Ketogenic Supplements
KetoneAid has concocted two forms of ketone supplementation to be used for either performance enhancement or as a substitute for ethyl-alcohol. On their website, KetoneAid differentiates between all the uses for these supplements and their associated protocols. Whether you are using these products for sleep, mental acuity, jet lag, or sports performance–KetoneAid has the protocol –> https://www.ketoneaid.com/protocol/

Ketone Salts vs. Ketone Esters

Ketones esters (KE4) have shown to improve mitochondrial function and are currently used to enhance functional performance. Drinking ketone esters is shown to decrease appetite through ghrelin suppression (Stubbs et. al, 2018). Oral consumption of a ketone ester can acutely increase circulating βHB concentrations as high as 5 mM in healthy adults (Margolis & O’Fallon, 2020). Remember, βHB is an energy alternative to carbohydrates. Ketone ester intake can protect against endurance training‐induced overreaching (Poffé, Ramaekers, Van Thienen & Hespel, 2019) and has been used widely by high performance athletes like Greg Henderson in the Tour de France. Henderson’s supplementation of ketone esters has transformed his cycling performance to be 15% faster than baseline, according to Frank Llosa.
Ketone esters have shown promising results with usage before, during, and after performance. Use code ANDRESKETONES for Free Shipping with your purchase of KE4.
Ketone salts (KE1) are a ketone ester blend with 2G of added salts. Innovations in ketone supplementation have led manufacturers to add salt into the solution to decrease “Keto-flu” symptoms because of the root cause being hyponatremia. KE1 is a freeform acid with added bases to be digestible for the human gut. KetoneAid’s KE1 solution is both non-racemic and caffeine free, meaning its ketone bioavailability is accurately reflective and the focused state is different from that of the stimulation felt by caffeine.

Hard Ketones (R 1,3) are KetoneAid’s newest blend of the first ever non-ethanol alcohol. R 1, 3 Hard Ketone Seltzer is 1/2 of the Ketone Ester molecule. Ketone ester is D-BHB attached to this same R 1,3 BD. When Ketone Ester is consumed it enters the bloodstream and it breaks into 2 parts: D-BHB and R 1,3 BD. R13 is not designed for performance enhancement and elicits more relaxed states. Although this is an alternative to alcohol, heavy machinery should not be operated. The metabolites of Hard Ketones do not produce the puffy, hangover effects that acetaldehyde produces after consuming ethyl alcohol. Use code ANDRESR13 for 15% off your purchase of Hard Ketones (must be 21+ years to purchase).
Warnings
Reported side effects of ketone supplementations include flatulence, nausea, diarrhea, constipation, vomiting, abdominal distress, and abdominal pain (Clarke et. al, 2012). Consumption of KetoneAids is best done under supervision of a health coach. KetoneAid is not FDA approved. To view available KYP coaches click here. Ketosis must be conquered with adequate electrolyte balance, water consumption, and sunlight exposure in order to reap the maximum benefit. KnowYourPhysio is committed to providing biohackers with the required scientific knowledge behind these lifestyle practices.
Actionable Steps
- Taper your carbohydrate intake to <50 G/day to suppress insulin release
- Increase intake of fatty foods
- Eggs
- Fish
- Nuts/seeds
- Avocados
- Full – fat dairy
- Mayonnaise
- Herbs/spices
- Gradually elongate the length of your fast
- HIIT training
- Try KE4
References
Abdul Kadir, A., Clarke, K., & Evans, R. D. (2020). Cardiac ketone body metabolism. Biochimica et biophysica acta. Molecular basis of disease, 1866(6), 165739. https://doi.org/10.1016/j.bbadis.2020.165739
Acharya, P., Acharya, C., Thongprayoon, C., Hansrivijit, P., Kanduri, S. R., Kovvuru, K., Medaura, J., Vaitla, P., Garcia Anton, D. F., Mekraksakit, P., Pattharanitima, P., Bathini, T., & Cheungpasitporn, W. (2021). Incidence and Characteristics of Kidney Stones in Patients on Ketogenic Diet: A Systematic Review and Meta-Analysis. Diseases (Basel, Switzerland), 9(2), 39. https://doi.org/10.3390/diseases9020039
Altayyar, M., Nasser, J. A., Thomopoulos, D., & Bruneau, M., Jr (2022). The Implication of Physiological Ketosis on The Cognitive Brain: A Narrative Review. Nutrients, 14(3), 513. https://doi.org/10.3390/nu14030513
Armstrong, L. E., & Johnson, E. C. (2018). Water Intake, Water Balance, and the Elusive Daily Water Requirement. Nutrients, 10(12), 1928. https://doi.org/10.3390/nu10121928
Clarke K, Tchabanenko K, Pawlosky R, Carter E, Todd King M, Musa-Veloso K, Ho M, Roberts A, Robertson J, Vanitallie TB et al. .. Kinetics, safety and tolerability of (R)-3-hydroxybutyl (R)-3-hydroxybutyrate in healthy adult subjects. Regul Toxicol Pharmacol. 2012;63(3):401–8.
Condon, K. J., & Sabatini, D. M. (2019). Nutrient regulation of mTORC1 at a glance. Journal of cell science, 132(21), jcs222570. https://doi.org/10.1242/jcs.222570
Cvijetic, S. (2021, February 11). What are brain waves (Theta, Delta, Alpha, beta brain waves)? what is brainwave entrainment? HubPages. Retrieved March 22, 2022, from https://discover.hubpages.com/education/What-are-Brain-Waves-Theta-Delta-Alpha-Beta-brain-waves-What-is-brainwave-entrainment
Dikic, I., & Elazar, Z. (2018). Mechanism and medical implications of mammalian autophagy. Nature reviews. Molecular cell biology, 19(6), 349–364. https://doi.org/10.1038/s41580-018-0003-4
DiNicolantonio, J. J., O’Keefe, J. H., & Wilson, W. L. (2018). Sugar addiction: is it real? A narrative review. British journal of sports medicine, 52(14), 910–913. https://doi.org/10.1136/bjsports-2017-097971
Evans, M., Cogan, K. E., & Egan, B. (2017). Metabolism of ketone bodies during exercise and training: physiological basis for exogenous supplementation. The Journal of physiology, 595(9), 2857–2871. https://doi.org/10.1113/JP273185
Freeman JM, Vining EPG, Pillas DJ, Pyzik PL, Casey JC, Kelly MT (1998) The efficacy of the ketogenic diet—1998: a prospective evaluation of intervention in 150 children. Pediatrics 102(Dec):1358–63 Freeman RS, Barone MC (2005) Targeting hypoxia inducible factor (HIF) as a therapeutic strategy for CNS disorders. Curr Drug Targets CNS Neurol Disord 4:85–92
Gao, D., Long, S., Yang, H., Cheng, Y., Guo, S., Yu, Y., Liu, T., Dong, L., Lu, J., & Yao, D. (2020). SWS Brain-Wave Music May Improve the Quality of Sleep: An EEG Study. Frontiers in neuroscience, 14, 67. https://doi.org/10.3389/fnins.2020.00067
Jensen, N. J., Wodschow, H. Z., Nilsson, M., & Rungby, J. (2020). Effects of Ketone Bodies on Brain Metabolism and Function in Neurodegenerative Diseases. International journal of molecular sciences, 21(22), 8767. https://doi.org/10.3390/ijms21228767
Katsiki, N., Doumas, M., & Mikhailidis, D. P. (2016). Lipids, Statins and Heart Failure: An Update. Current pharmaceutical design, 22(31), 4796–4806. https://doi.org/10.2174/1381612822666160701073452
Ma, Q., Fang, L., Su, R., Ma, L., Xie, G., & Cheng, Y. (2018). Uric acid stones, clinical manifestations and therapeutic considerations. Postgraduate medical journal, 94(1114), 458–462. https://doi.org/10.1136/postgradmedj-2017-135332
Margolis, L. M., & O’Fallon, K. S. (2020). Utility of Ketone Supplementation to Enhance Physical Performance: A Systematic Review. Advances in nutrition (Bethesda, Md.), 11(2), 412–419. https://doi.org/10.1093/advances/nmz104
Napoleão, A., Fernandes, L., Miranda, C., & Marum, A. P. (2021). Effects of Calorie Restriction on Health Span and Insulin Resistance: Classic Calorie Restriction Diet vs. Ketosis-Inducing Diet. Nutrients, 13(4), 1302. https://doi.org/10.3390/nu13041302
Peschke, E., Bähr, I., & Mühlbauer, E. (2013). Melatonin and pancreatic islets: interrelationships between melatonin, insulin and glucagon. International journal of molecular sciences, 14(4), 6981–7015. https://doi.org/10.3390/ijms14046981
Poffé, C., Ramaekers, M., Van Thienen, R., & Hespel, P. (2019). Ketone ester supplementation blunts overreaching symptoms during endurance training overload. The Journal of physiology, 597(12), 3009–3027. https://doi.org/10.1113/JP277831
Porth, C. M. (2011). Essentials of Pathophysiology: Concepts of Altered Health States (4th ed.). Wolters Kluwer.
Prince, A., Zhang, Y., Croniger, C., & Puchowicz, M. (2013). Oxidative metabolism: glucose versus ketones. Advances in experimental medicine and biology, 789, 323–328. https://doi.org/10.1007/978-1-4614-7411-1_43
Stubbs, B. J., Cox, P. J., Evans, R. D., Cyranka, M., Clarke, K., & de Wet, H. (2018). A Ketone Ester Drink Lowers Human Ghrelin and Appetite. Obesity (Silver Spring, Md.), 26(2), 269–273. https://doi.org/10.1002/oby.22051
Tan, D. X., Xu, B., Zhou, X., & Reiter, R. J. (2018). Pineal Calcification, Melatonin Production, Aging, Associated Health Consequences and Rejuvenation of the Pineal Gland. Molecules (Basel, Switzerland), 23(2), 301. https://doi.org/10.3390/molecules23020301
Yamaguchi O. (2019). Autophagy in the Heart. Circulation journal : official journal of the Japanese Circulation Society, 83(4), 697–704. https://doi.org/10.1253/circj.CJ-18-1065
Yılmaz, Ü., Nalbantoğlu, Ö., Güzin, Y., Edizer, S., Akışin, Z., Pekuz, S., Kırkgöz, H. H., Yavuz, M., Ünalp, A., & Özkan, B. (2021). The effect of ketogenic diet on thyroid functions in children with drug-resistant epilepsy. Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology, 42(12), 5261–5269. https://doi.org/10.1007/s10072-021-05225-y
Effect of ketone esters in parkinson’s disease – full text view. Full Text View – ClinicalTrials.gov. (n.d.). Retrieved March 22, 2022, from https://clinicaltrials.gov/ct2/show/NCT04477161
Ketone Body Imagine:
M.S. Muyyarikkandy, M. McLeod, M. Maguire, R. Mahar, N. Kattapuram, C. Zhang, C. Surugihalli1, V. Muralidan1, K. Vavilikolanu1, C.E. Mathews2, M.E. Merritt2, and N.E. Sunny. (2021). Using magnetic resonance to probe lipid synthesis in response to ketogenic diet – maglab. The National High Magnetic Field Laboratory. Retrieved from https://nationalmaglab.org/user-facilities/nmr-mri/publications-nmr-mri/highlights-amris/lipid-synthesis-ketogenic-diet
Liver Metabolism Image:
Selvaraj, S., Kelly, D. P., & Margulies, K. B. (2020). Implications of Altered Ketone Metabolism and Therapeutic Ketosis in Heart Failure. Circulation, 141(22), 1800–1812. https://doi.org/10.1161/CIRCULATIONAHA.119.045033
Picture of mtorc1:
Parzych, K. R., & Klionsky, D. J. (2014). An overview of autophagy: morphology, mechanism, and regulation. Antioxidants & redox signaling, 20(3), 460–473. https://doi.org/10.1089/ars.2013.5371
Sleep wave picture:
Chitimus, D. M., Popescu, M. R., Voiculescu, S. E., Panaitescu, A. M., Pavel, B., Zagrean, L., & Zagrean, A. M. (2020). Melatonin’s Impact on Antioxidative and Anti-Inflammatory Reprogramming in Homeostasis and Disease. Biomolecules, 10(9), 1211. https://doi.org/10.3390/biom10091211







