Podcast 34 with Kayla Osterhoff, MPH, PhD
Joining us in conversation today is Kayla Osterhoff, who teaches us that it’s never too late or too early for women to learn about their biorhythm, and live a healthier, more empowered life because of it. Tune in to hear about Kayla’s academic and professional background and the personal experiences that motivated her to focus on women’s health. She describes the female biorhythm as the pace that the female body is set to, and tells us why, even as a health scientist, she didn’t know how to be healthy; all the research was based on male biology! Kayla tells us why she has chosen to work independently with private partners, rather than pursuing a career with the government, and tells us the difference between the female hormonal cycle and the female biorhythm, before teaching us about the four phases of the biorhythm cycle, all with one shared key: to go with the flow of your body. She considers the female biorhythm to be a huge biohack that sets women apart for success and gives listeners some interesting tips on how to optimize each cycle and see results. We touch on the benefits and dangers of a ketogenic diet and talk about the technology Kayla has patented in the past year to go live in 2022. Kayla also tells us why biohacking is so much more important for women than it is for men. Thanks for listening! We hope you gained insight into your physiology today.
____________________________________________________________
Science that’s Sexy
By: Ariel Kamen, BSN, RN
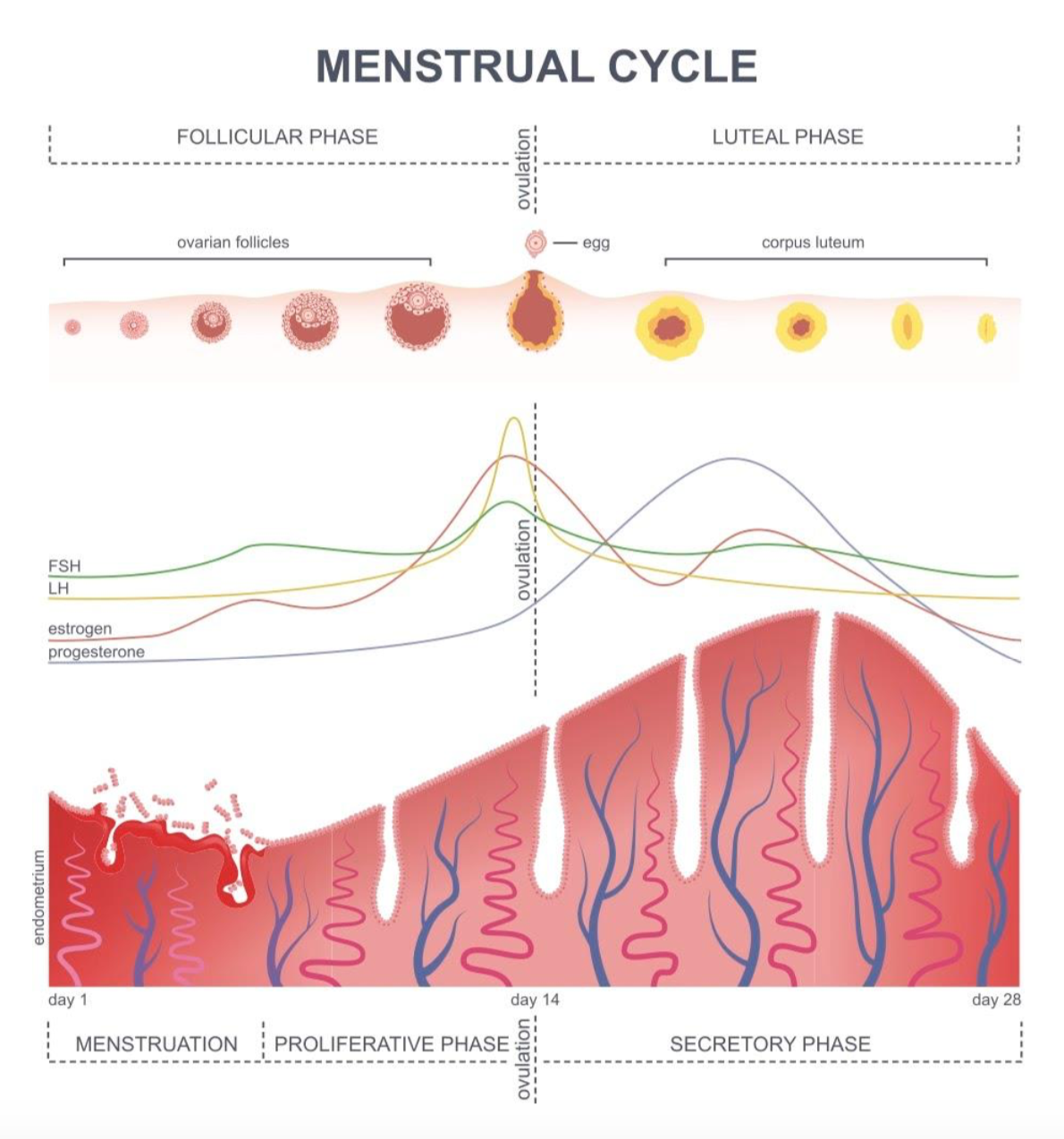
Women are vital to humanity’s progression. Each month there is opportunity for growth, not only of cells but ideas, relationships, and progress as well. Over the course of 28 days, the peaks and troughs of sex steroid hormones allow women to function at ever-changing energy levels. In Episode 34 with Dr. Kayla Osterhoff, we learn to go with our flow and absorb all things Female Biorhythm. Over the course of 28 days, the ability of women to shed, plant, bloom, and grow has allowed humanity to expand for generations. Birth rates, maternal mortality, and formula shortages are serious global concerns. At the core, we discover the Female Biorhythm, a synthesis of the female menstrual cycle and explanations of each day on a hormonal level.
Sex Steroid Hormones
Hormones are a form of energy for the body. Without sex hormones, we are soft and exhausted; with them we are hard and aroused. There are vast amounts of hormones in the body, but for the sake of reproduction, we will focus on a few. Estrogen and progesterone may be familiar to some.
Most of the enzymes involved in steroidogenesis belong to the family of CYP450. (Guiochon-Mantel, Milgrom & Schaison, 1999).
FSH
LH
Estrogen
Estrogen deficiency is detrimental to many wound-healing processes, notably inflammation and re-granulation, while exogenous estrogen treatment widely reverses these effects. Over recent decades, many of the molecular and cellular correlates to estrogen’s beneficial effect on normal skin homeostasis and wound healing have been reported (Wilkinson & Hardman, 2017).
Estrogen synthesis is directed by FSH, and only small amounts of LH are needed to amplify the follicular estrogenic potential (Shoham, & Schachter, 1996).
Progesterone
Estradiol (E2) is women’s dominant ‘bone hormone’ since it is essential for development of adolescent peak bone mineral density (BMD)
Both estradiol (E2, ‘women’s hormone’) and progesterone (P4), E2’s ovarian partner hormone, play essential roles in bone balance. E2 slows bone resorption and P4 stimulates bone formation (Prior, 2018).
progesterone significantly influences normal mammary growth and differentiation (Speroff, 1999).
Progesterone, the natural progestin, is a major gonadal hormone that is synthesized primarily by the ovary in the female, and the testes and adrenal cortex in the male (Singh & Su, 2013).
Testosterone
Know Your Physio’s expert, Kayla Osterhoff, MPH and PhD in neuropsychophysiology, takes Andrés through the flow of The Female Biorhythm and tells us how we can best enhance our performance depending on our time of the month. You can learn more about Dr. Osterhoff’s 8 week course that dives into all things female biorhythm at https://www.biocurious.co/.
History of Women in Research
In 1977, the FDA Guidance General Considerations for the Clinical Evaluation of Drugs excluded women of childbearing potential from participating in Phase I and early Phase II clinical trials. Until 1993, the FDA Guidance Study and Evaluation of Gender Differences in the Clinical Evaluation of Drugs withdrew restrictions outlined in the 1977 guidance on the participation of women of childbearing potential in early clinical trials (Commissioner, 2021).
For 16 years there were zero clinical pharmacology studies and early therapeutic studies about the female body. There is barely research covering pharmacokinetics and pharmacodynamics in women, or even analysis of safety and efficacy by sex. Now, 29 years after the restrictions have been withdrawn, there is still an information void in The Female Biorhythm.
What is the Female Biorhythm?
The Female Biorhythm describes the physiological reverberation of the female body over the course of a month. Kayla spent six years painting a physiological picture of the female body and deduced how to function optimally during each Menstrual Phase. Learning about The Female Biorhythm offers women a way to build rapport with their own bodies as the month goes on.
Barriers seen in personal training As a professional athlete and health scientist at the CDC, Kayla shares her story “so other women do not get stuck in the treacherous burnout cycle.” In reflection, she says, “every day I was consistent, but I was not paying attention to my body’s needs throughout the month.” From here, Kayla began to intimately study the rise and fall of hormones in female physiology and the bodily changes over the 28 day Menstrual cycle.
So what are those physical changes that occur over the month?
Shed Phase: Days 1-5 (Menstruation)
The first five days of menstruation are characterized as the active period. Kayla calls this the “Shed phase.” Let’s see why:
Estrogen and Progesterone are tanked, out of amo, low on fuel. In our brain, these hormones are present in high densities in the parts of the brain responsible for leadership (Matthews & Tye, 2019).
- Prefrontal cortex – decision making
- Hypothalamus – emotional intelligence
- Hippocampus – memory consolidation
In bioenergetics, estrogen plays a role in synthesizing ATP (Kim et. al, 2021).The body is literally shedding what no longer serves the female body.
[Readers note: not all females experience an active phase, for more information contact I[email protected]]
It is during these three to five days that estrogen and progesterone are at their lowest level; as a result, the body slows down and produces less energy. Women naturally have lower energy levels than men, but trough levels occur during menstruation. Additionally, a cognitive shift occurs when the aforementioned hormones are low (Rettberg, Yao & Brinton, 2014). The female may experience enhanced empathy, intuition, and her ability to assess is heightened. To best integrate this into the physical world, these early days are the best time to cut back on stimulants. Better said, it is not optimal to drink extra coffee during these 3 to 5 days, depending on the individual, to compensate for the body being naturally drained.
Plant Phase: Days 6-12 (Follicular Phase)
Once the active period ends, the body enters what Kayla calls the “Plant Phase… like planting the seeds for success.” Within the body, estrogen is steadily rising to a peak. As buildup progresses, the body produces more ATP (energy currency for the body), metabolism increases, and there is greater presence of the neurotransmitters; serotonin, norepinephrine, epinephrine, and dopamine (Monis & Tetrokalashvili, 2021). A cognitive shift occurs over these next several days, where the female has greater navigational ability and is able to think strategically. Kayla mentions that this is the best time for ladies to begin putting their plans into action.
Bloom Phase: Days 13-15 (Ovulation)
As we journey along this 28 day cycle, ovulation is the halfway biomarker. Since this is only a two to three day occurrence, Kayla describes this time to be more of a phase shift over 1 to 3 days, rather than a phase of itself. Coined name “Bloom Phase” is when females begin to feel energized again, like they have more charismatic influence, can work longer hours, and are more outwardly expressive (Holesh, Bass & Lord, 2021). The cognitive shift that occurs during ovulation makes it a great time to socialize and network. For the fellas, knowing the days when your partner will be the most energized can be a helpful relationship tool, but please be conscious that the body becomes more vulnerable to fertilization during this phase (Robker, Hennebold, & Russell, 2018). In other words, use protection 😉 !
Grow Phase: Days 16-28 (Luteal Phase)
After ovulation, Kayla names this next set of days as the “Grow Phase.” This is the time period when progesterone is rising and the brain grows too as a result. It is necessary to understand that hormones are not isolated molecules and are dispatched throughout the body. For all the “neuro nerds,” says Kayla, “lets dive a little deeper into the neurophysiology” surrounding the increase in progesterone: 
- Brain derived neurotrophic factor (BDNF) increases which also increases neural plasticity. This refers to the shape, neural pathways, and ability to change behavior in the brain. Neurogenesis is also on the rise, thus the brain has a higher mental acuity and ability to build new neurons. Because of this, the “Grow Phase” is the best time to kick junky habits and introduce others (Dominguez, Cho, Zhang, Neal & Foster, 2011).
- Neurotransmitter, GABA becomes more available which enhances parasympathetic functions and allows for the brain to enter into deep, delta brain wave sleep. Deep sleep is important because this is when memory consolidation occurs. To benefit from these cool neuro functions, sleep must be prioritized from days 16 to 28 (Gottesmann, 2002).
Sex Hormones, Brain and Behavior
Sex hormones, such as estrogens, progesterone, and testosterone influence cognitive functioning and have been at the basis of studies examining sex differences in behavior for decades (Le, 2020). There are two broad phases of the menstrual cycle, the follicular phase and the luteal phase. The follicular phase begins on day 1 of active bleeding and ends with ovulation, followed by the luteal phase until menses occurs again, when the cycle repeats.
Both estrogen receptors (ER-α and ER-β) and progesterone receptors (PR-A and PR-B) have been found in cognitively-relevant brain regions, such as the amygdala, hippocampus, and the prefrontal cortex (Hara, 2014). Both hormones are lipophilic, which means they can pass through the blood–brain barrier and bind to foods high in dietary fats.
Alignment with the natural rise and fall of sex hormones over the course of 28 days can allow females to best prepare themselves for the cognition they can endure depending on the concentration of sex hormones throughout the Female Biorhythm.
Studies in shift workers show that cognitive lapses and errors are more prevalent during the follicular phase of the cycle. On the other hand, concentration and cognition dominate the luteal phase (cite).
Childbirth
The placenta plays a vital role in fetal development during pregnancy. Dysfunction of the placenta can be caused by oxidative stress and can lead to abnormal fetal development. Preventing oxidative stress of the placenta is thus an important measure to ensure positive birth outcomes. Research shows that tryptophan and its metabolites can efficiently clean free radicals (including the reactive oxygen species and activated chlorine).
Xu, K., Liu, G., & Fu, C. (2018). The Tryptophan Pathway Targeting Antioxidant Capacity in the Placenta. Oxidative medicine and cellular longevity, 2018, 1054797. https://doi.org/10.1155/2018/1054797
Menopause
Menopause, denoted by a rapid decline in serum sex steroid levels, accelerates biological ageing across the body’s tissues (Wilkinson & Hardman, 2017).
Actionable Steps:
- Track your menstrual cycle using a calendar or the Clue Period & Cycle Tracker App
- Consider if you take oral contraceptives or have an IUD
- If yes, this may change your female biorhythm by hiding the active bleeding period
- Stay away from caffeinated beverages during your active period. Because energy levels are the lowest during these 5 days, overcompensating your energy levels using caffeine puts more stress on your body
- Prioritize sleep during the last two weeks after ovulation (day 14)
Dr. Osterhoff says, “over the course of a month females have a menstrual cycle but when you zoom out, you get the Female Biorhythm. This integrates the physical symptoms throughout the menstrual cycle, and the neuropsychological occurrences over the month.” Go with your flow & know your physio!
Resources
Brinton R.D., Thompson R.F., Foy M.R., Baudry M., Wang J., Finch C.E., Morgan T.E., Pike C.J., Mack W.J., Stanczyk F.Z., et al. Progesterone receptors: Form and function in brain. Front. Neuroendocrinol. 2008;29:313–339. doi: 10.1016/j.yfrne.2008.02.001.
Commissioner, O. (2021). Regulations, guidance, and reports related to women’s health. U.S. Food and Drug Administration. Retrieved January 27, 2022, from https://www.fda.gov/science-research/womens-health-research/regulations-guidance-and-reports-related-womens-health
Dominguez, M. A., Cho, N., Zhang, B., Neal, M. S., & Foster, W. G. (2011). Brain-derived neurotrophic factor expression in granulosa lutein cells. Reproductive biomedicine online, 22(1), 17–24. https://doi.org/10.1016/j.rbmo.2010.09.001
Gottesmann C. (2002). GABA mechanisms and sleep. Neuroscience, 111(2), 231–239. https://doi.org/10.1016/s0306-4522(02)00034-9
Guiochon-Mantel, A., Milgrom, E., & Schaison, G. (1999). Biosynthèse et récepteurs des estrogènes [Estrogen biosynthesis and receptors]. Annales d’endocrinologie, 60(5), 381–391.
Hara Y., Waters E.M., McEwen B.S., Morrison J.H. (2014). Estrogen Effects on Cognitive and Synaptic Health Over the Lifecourse. Physiol. Rev. 2015;95:785–807. doi: 10.1152/physrev.00036.
Holesh, J. E., Bass, A. N., & Lord, M. (2021). Physiology, Ovulation. In StatPearls. StatPearls Publishing.
Kim, S., Lee, J. Y., Shin, S. G., Kim, J. K., Silwal, P., Kim, Y. J., Shin, N. R., Kim, P. S., Won, M., Lee, S. H., Kim, S. Y., Sasai, M., Yamamoto, M., Kim, J. M., Bae, J. W., & Jo, E. K. (2021). ESRRA (estrogen related receptor alpha) is a critical regulator of intestinal homeostasis through activation of autophagic flux via gut microbiota. Autophagy, 17(10), 2856–2875. https://doi.org/10.1080/15548627.2020.1847460
Le, J., Thomas, N., & Gurvich, C. (2020). Cognition, The Menstrual Cycle, and Premenstrual Disorders: A Review. Brain sciences, 10(4), 198. https://doi.org/10.3390/brainsci10040198
Matthews, G. A., & Tye, K. M. (2019). Neural mechanisms of social homeostasis. Annals of the New York Academy of Sciences, 1457(1), 5–25. https://doi.org/10.1111/nyas.14016
Monis, C. N., & Tetrokalashvili, M. (2021). Menstrual Cycle Proliferative And Follicular Phase. In StatPearls. StatPearls Publishing.
Rettberg, J. R., Yao, J., & Brinton, R. D. (2014). Estrogen: a master regulator of bioenergetic systems in the brain and body. Frontiers in neuroendocrinology, 35(1), 8–30. https://doi.org/10.1016/j.yfrne.2013.08.001
Robker, R. L., Hennebold, J. D., & Russell, D. L. (2018). Coordination of Ovulation and Oocyte Maturation: A Good Egg at the Right Time. Endocrinology, 159(9), 3209–3218. https://doi.org/10.1210/en.2018-00485
Shoham, Z., & Schachter, M. (1996). Estrogen biosynthesis–regulation, action, remote effects, and value of monitoring in ovarian stimulation cycles. Fertility and sterility, 65(4), 687–701. https://doi.org/10.1016/s0015-0282(16)58197-7
Singh, M., & Su, C. (2013). Progesterone, brain-derived neurotrophic factor and neuroprotection. Neuroscience, 239, 84–91. https://doi.org/10.1016/j.neuroscience.2012.09.056
Speroff L. (1999). Role of progesterone in normal breast physiology. The Journal of reproductive medicine, 44(2 Suppl), 172–179.
Sundström Poromaa I., Gingnell M. Menstrual cycle influence on cognitive function and emotion processing—From a reproductive perspective. Front. Neurosci. 2014;8:8. doi: 10.3389/fnins.2014.00380.
Picture 1: Your Spark is Light by Dr. Courtney Hunt
Picture 2: https://www.rcsb.org/3d-view/1B8M
Picture 3: https://www.rcsb.org/3d-view/4MS3/1
Prior J. C. (2018). Progesterone for the prevention and treatment of osteoporosis in women. Climacteric : the journal of the International Menopause Society, 21(4), 366–374. https://doi.org/10.1080/13697137.2018.1467400
Wilkinson, H. N., & Hardman, M. J. (2017). The role of estrogen in cutaneous ageing and repair. Maturitas, 103, 60–64. https://doi.org/10.1016/j.maturitas.2017.06.026